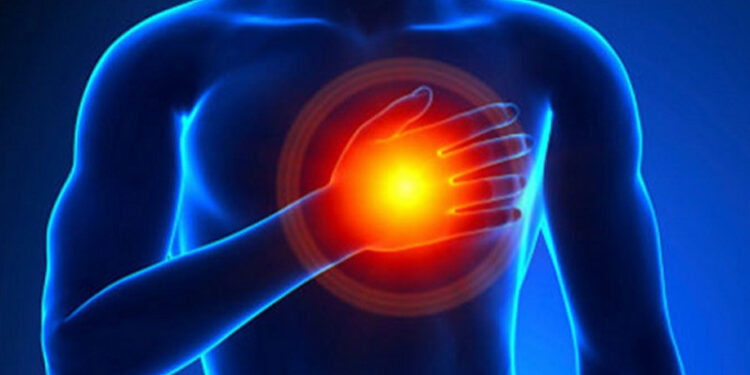
Experience with “chest pain left side“ is often terrifying, but it’s important to know that most cases in healthy individuals under 50 are not heart attacks. Common non-cardiac causes include acid reflux, muscle strain, or costochondritis (inflammation of the rib cartilage). However, if the pain is crushing, radiates to your arm or jaw, or is accompanied by cold sweats and nausea, it is a medical emergency.
**The short answer:** Left-sided chest pain can stem from the heart, lungs, digestive system, muscles, nerves, or anxiety. Cardiac causes must be ruled out first. If the pain is accompanied by pressure, radiating pain to the arm or jaw, shortness of breath, sweating, or nausea – call emergency services immediately. For isolated, sharp, or position-related pain in a healthy person, non-cardiac causes are far more likely.
—
⚠️ Call Emergency Services Immediately If You Have:
- Crushing, squeezing, or heavy pressure in the chest
- Pain radiating to the left arm, jaw, neck, or back
- Shortness of breath alongside chest pain
- Cold sweats, nausea, or vomiting
- Sudden dizziness or feeling faint
- Palpitations with chest discomfort
- Pain that persists more than 5 minutes
These symptoms – especially in combination – may indicate a heart attack or other cardiac emergency. Do not drive yourself. Do not wait to see if it improves. Call for help.
—
Common Causes of Left-Sided Chest Pain
| Cause | Type | Pain Character | Other Clues |
|—|—|—|—|
| Heart attack (MI) | Cardiac | Pressure, squeezing, heaviness | Radiates to arm/jaw, sweating, nausea |
| Angina | Cardiac | Tightness, pressure | Triggered by exertion, relieved by rest |
| Pericarditis | Cardiac | Sharp, worse lying down | Improved sitting forward, recent illness |
| Costochondritis | Musculoskeletal | Sharp, tender to touch | Reproducible by pressing on ribcage |
| GERD / acid reflux | Digestive | Burning, worse after eating | Heartburn, sour taste, lying flat worsens it |
| Pleuritis (pleurisy) | Pulmonary | Sharp, worse with breathing | Cough, recent respiratory infection |
| Pulmonary embolism | Pulmonary | Sudden sharp, worse breathing | Shortness of breath, recent travel or immobility |
| Muscle strain | Musculoskeletal | Aching, tender area | Recent physical exertion or awkward movement |
| Anxiety / panic attack | Psychological | Tightness, sharp, or variable | Palpitations, shortness of breath, fear |
| Precordial catch syndrome | Benign | Brief sharp stab | Young person, resolves in minutes, at rest |
| Shingles (early) | Neurological | Burning, one-sided | May precede rash by 1-3 days |
—
Cardiac Causes – What to Know
Heart Attack (Myocardial Infarction)
A heart attack occurs when blood supply to part of the heart muscle is blocked, usually by a clot in a coronary artery. The classic presentation is chest pressure radiating to the left arm or jaw, with sweating and nausea – but symptoms vary significantly, especially in women and diabetics, who more often present with fatigue, breathlessness, or back pain rather than classic chest pressure.
Angina
Stable angina is chest tightness triggered by exertion and relieved by rest or nitroglycerin. Unstable angina occurs at rest or with minimal activity and represents a medical emergency. Both require urgent evaluation.
Pericarditis
Inflammation of the sac around the heart, often following a viral illness. The pain is typically sharp, worse when lying flat, and improved when sitting forward. It needs medical treatment but is rarely immediately life-threatening.
—
Non-Cardiac Causes – More Common Than Most People Think
Costochondritis
Inflammation of the cartilage connecting the ribs to the sternum. It’s one of the most common causes of chest pain seen in emergency rooms – and one of the most benign. The defining sign: pressing on the affected area reproduces the pain. Treatment is anti-inflammatories, rest, and time.
GERD / Acid Reflux
Gastroesophageal reflux disease can cause chest burning that mimics cardiac pain closely enough that it’s sometimes called “cardiac non-cardiac chest pain.” Clues include burning rather than pressure, worsening after meals or lying down, and a sour or bitter taste in the mouth.
Anxiety and Panic Attacks
Anxiety-related chest pain is real, physical, and often indistinguishable from cardiac pain in the moment. It’s often accompanied by rapid heart rate, shortness of breath, dizziness, and a sense of impending doom. The key is ruling out cardiac causes first – then addressing the anxiety.
Pleurisy
Inflammation of the lining around the lungs, often following infection. The pain is sharp, worsens sharply with each breath, and may have associated cough or fever.
Pulmonary Embolism
A blood clot in the lung. This is a medical emergency. Sudden sharp chest pain with unexplained shortness of breath, especially after a long flight, surgery, or period of immobility, warrants immediate emergency care.
—
How Doctors Evaluate Chest Pain
When you arrive at a clinic or emergency department with chest pain, the evaluation is systematic:
| Test | What It Checks |
|—|—|
| ECG (EKG) | Electrical activity of the heart – detects heart attack, arrhythmia |
| Troponin blood test | Protein released when heart muscle is damaged – key heart attack marker |
| Chest X-ray | Lung conditions, heart size, rib abnormalities |
| CT pulmonary angiography | Rules out pulmonary embolism |
| Echocardiogram | Heart structure and function |
| Physical exam | Reproducing pain by palpation helps identify musculoskeletal causes |
—
Final Thought
Left-sided chest pain is something you take seriously – but not something you panic about before getting assessed. The range of causes spans from completely harmless (precordial catch syndrome, costochondritis) to immediately life-threatening (heart attack, pulmonary embolism).
The rule is simple: if it could be cardiac, get evaluated. Don’t self-diagnose, don’t wait it out if symptoms are severe, and don’t let embarrassment stop you from calling for help.
An ECG takes 5 minutes. A proper evaluation takes an hour. Your life is worth both.